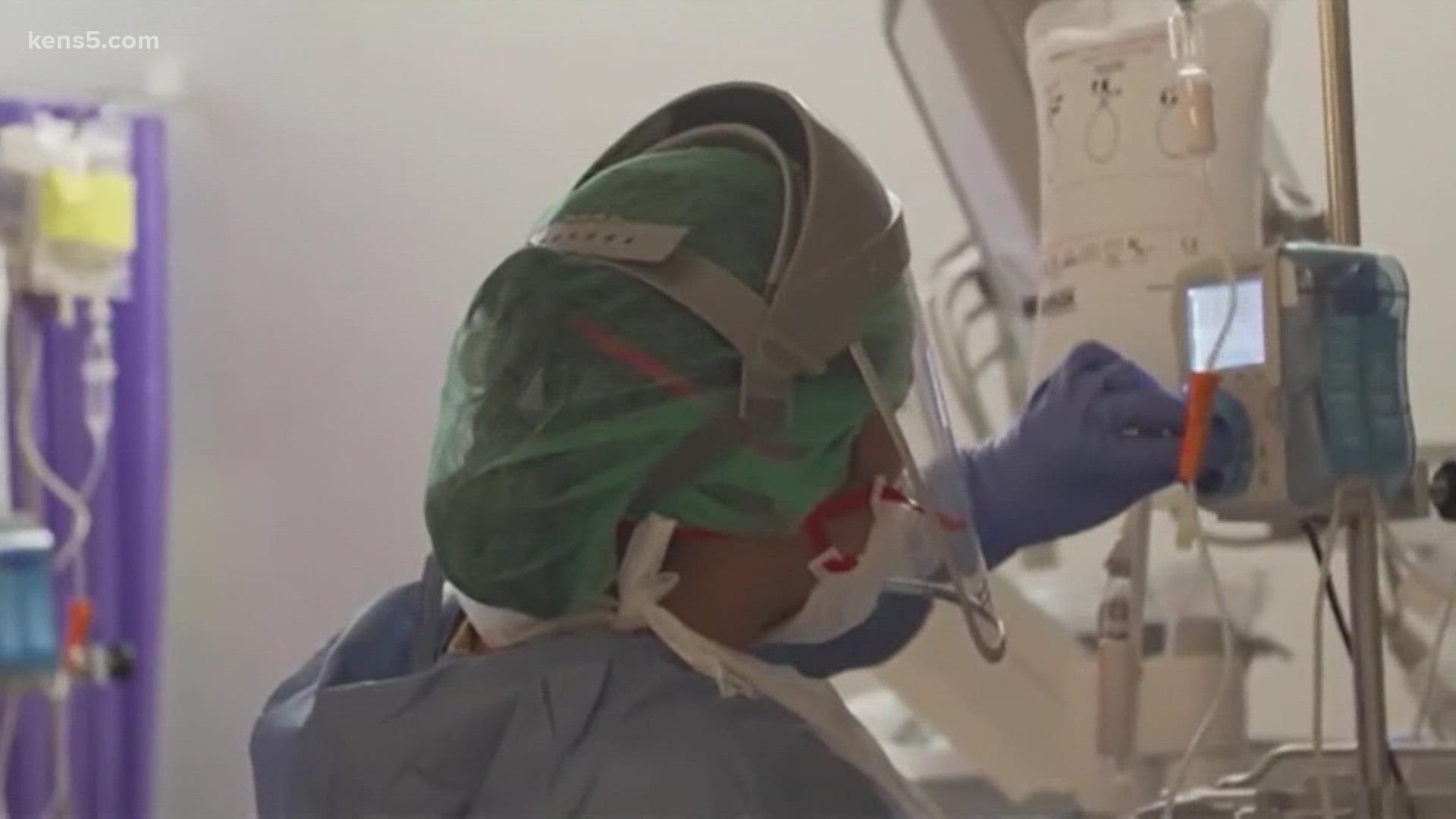
SAN ANTONIO — Treatment for COVID-19 has evolved, producing better outcomes for hospitalized patients in the 20 months since doctors first detected the disease in the United States.
Patients suffering from COVID-19 now benefit from new medicines and methods for care, though the vaccine remains the most effective defense against the disease.
"We've done a good job of reading the patterns," said Dr. Duane Hospenthal, Baptist Health Systems's lead infectious disease physician. "The outcomes in our sickest are better. They're certainly not great, and not everybody survives, but they're better."
Remdesivir is among the first medicines scientists approved that can prevent moderate sickness from becoming severe. It is an anti-viral medication used for patients who have just checked into the hospital and require some oxygen
"Think of it like TamiFlu," Hospenthal said. "It's not that it's going to cure the COVID, but, if given at the right time, it may decrease the viral load enough to give you a benefit that allows your immune system to get you through."
The drug is not especially effective for patients whose disease has progressed enough to require a ventilator for breathing, for example.
Those sickest patients may benefit from a steroid that can dampen the body's response, effectively preventing the immune system from overreacting to COVID-19.
A steroid administered too early may harm the patient's ability to fight off the virus on their own, though.
Patients also take anti-inflammatories and medicine that can prevent blood-clotting, Hospenthal said.
Supported mostly by anecdotal evidence, doctors aim to keep patients off mechanical ventilators for as long as possible. These machines execute the entire breathing process on a patient's behalf.
Hospenthal says doctors moved patients to ventilators more quickly at the onset of the pandemic. There was some concern, he says, that alternative oxygen delivery systems might spray the virus across the room and endanger hospital staff.
Today, doctors are more likely to put a patient with COVID-19 on a BiPap or high-flow oxygen machine before they use a ventilator. These devices were not commonly found outside intensive care units prior to the pandemic.
"Not everyone on high-flow or BiPap is in an ICU bed," Hospenthal said. "They are in the COVID wards and that allows us to take care of probably threefold or more, maybe not critically ill, but very, very sick patients."
In addition, doctors "prone" their patients on supplemental oxygen. This process allows air to move more freely through infected lungs.
Hospenthal says a sick person can do this at home, too, by lying on their stomach or side tilting forward.
"Just like the unified effort for HIV/AIDS, if enough resources and interest is there then we can move the science forward quicker," Hospenthal said, calling the scientific advances related to COVID-19 "remarkable."
Treatment for patients who do not yet need a hospital has also progressed. People who test positive for COVID-19 may have virus-fighting antibodies injected directly into their immune systems.
This is accomplished through a transfusion of convalescent plasma containing antibodies from a person who has already defeated COVID-19, or an injection of monoclonal antibodies created in a lab.
"We have seen that monoclonal antibodies have ben very effective in those that have taken a longer time to produce a response to COVID-19," said Dr. Nimesh Patel, medical director for Quality Urgent Care. "We want to give it to people who we've learned could progress to a severe disease."
Susceptible people include the elderly, or others with underlying health conditions like high-blood pressure or diabetes.
The therapy is also available to vaccinated people who've come down with a breakthrough infection or at-risk people who have asymptomatic infections, Patel said.
"Even though they feel fine, it might be something they might want to do," Patel said. "We've learned with COVID-19, you may feel fine one day and then all of a sudden your body will generate this response that can cause a progression we don't want to see."
The treatment is best administered as soon as possible, within 10 days of a positive test. Patel's Quality Urgent Care offers the therapy to the general public, though they must consult with one of their doctors first.
"It took a little bit of time, but it's still fascinating how quickly science was able to determine possible therapies," Patel said. "It shows that we have a common goal and a common interest. At the end of the day, we are humans and we do look out for each other."